Antimicrobials from human skin commensal bacteria protect against Staphylococcus aureus and are deficient in atopic dermatitis.
Nakatsuji T, Chen TH, Narala S, Chun KA, Two AM, Yun T, Shafiq F, Kotol PF, Bouslimani A, Melnik AV, Latif H, Kim JN, Lockhart A, Artis K, David G, Taylor P, Streib J, Dorrestein PC, Grier A, Gill SR, Zengler K, Hata TR, Leung DY, Gallo RL.
Sci Transl Med. 2017 Feb 22;9(378). pii: eaah4680. doi: 10.1126/scitranslmed.aah4680.
- The living organisms normally residing on the skin play a fundamental role in the maintenance of normal appearing skin. The “microbiome” contains a huge quantity and diversity of bacteria and coagulase negative Staphylococcus (CoNS) are one class of them. These comprise Staphylococcus Epidermidis and Hominis.
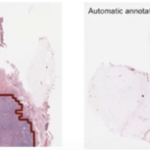
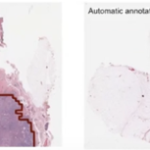
- This study shows that in contrast with normal skin, there is an inability in Atopic Dermatitis (AD) to prevent Staphylococcus Aureus (SA) colonization….due to absence of CoNS.
- CoNS presence is associated with Anti-microbial Peptides (AMP) production. This stops the colonization of SA.
- AD is colonized by SA and at the same time there is a deficiency of CoNS and AMP.
- these findings came from skin samples of healthy and AD subjects.
- The antibacterial action of was confirmed by reapplying CoNS on mice.
- Also reintroduction of antimicrobial CoNS strains to human subjects with AD decreased colonization by SA.
- Introducing AMPs: “These are essential immune defense molecules produced by neutrophils, paneth cells, mast cells, epithelial cells, and adipocytes. Because of their direct antimicrobial action, AMPs control growth of microorganisms that normally reside on epithelial surfaces, a community of microbes referred to as the “microbiome”. AMPs include canthelicidins, LL-37, b-defensin-2, and b-defensin-3.
To read the abstract of the article, click here: https://www.ncbi.nlm.nih.gov/pubmed/28228596
Article selected by Saurat JH, MD