What do you think about this study?
A treatment for severe nodular acne: a randomized investigator-blinded, controlled, noninferiority trial comparing fixed-dose adapalene/benzoyl peroxide plus doxycycline vs. oral isotretinoin (http://onlinelibrary.wiley.com/doi/10.1 … 13191/epdf).
For those of you who haven’t read it, it was an industry-sponsored trial comparing the most recent topical Epiduo (Adapalene/BPO) given together with Doxycycline against isotretinoin. The majority of authors are consultants, advisory board members or employees of Galderma.
Background
Oral isotretinoin (ISO) is the gold standard for severe nodular acne. However, as some patients are unwilling or unable to take, or are intolerant to, ISO, other options are needed.
Objectives
To compare efficacy and safety of oral ISO vs. doxycycline 200 mg plus adapalene 0?1%/benzoyl peroxide 2.5% gel (D+A/BPO) in severe nodular acne over 20 weeks.
Methods
This was a multicentre, randomized, controlled, noninferiority investiga- tor-blinded study involving 266 subjects.
Results
D+A/BPO showed a significantly earlier onset of action in reducing nodules, papules/pustules and total lesions at week 2. ISO was superior in reducing nodules (95?.6% vs. 88.7%), papules/pustules (95.2% vs. 79.6%) and total lesions (92.9% vs. 78.2%; all P < 0.01) at week 20. Half as many subjects for D+A/BPO compared with ISO had treatment-related, medically relevant adverse events (33 events in 18.0% of subjects vs. 73 in 33.8% of subjects, respectively). D+A/BPO was noninferior to ISO in the intent-to-treat population [95% confidence interval (CI) .2.7 to 20.8 (P = 0.13); 63.9% vs. 54.9% of subjects, respectively] and per- protocol population [95% CI 3.9–28.6 (P = 0.01); 74.3% vs. 58% of subjects, respectively), based on the composite efficacy/safety end point.
Conclusions
D+A/BPO showed a favourable composite efficacy/safety profile compared with ISO. This combination is an alternative to ISO in patients intolerant to, or unable or unwilling to take, oral ISO, and is an option for treatment of severe nodular acne.
This study has several limitations including, in my opinion, a potentially biased interpretation of the data.
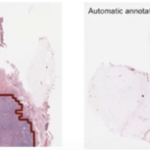
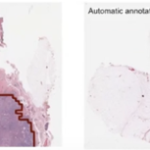
At the endpoint of the study, all relevant and achievable surrogates for acne intensity such as number of nodules, papules and pustules, total lesion counts, P. acnes fluorescence intensity and IGA (investigators global assessment) from baseline are clearly (and significant p < 0.05) better with isotretinoin than with D+A/BPO. Also, the curves are diverging towards stagnation in D+A/BPO and improvement in isotretinoin. Early on at 2 weeks however, the topical is a bit better in some measures, as might have been expected. The safety data is better with the D+A/BPO compared to isotretinoin.
The bias I perceived is introduced when the authors introduce a composite score of 16 safety measures and just 1 measure of efficacy (75% reduction of acne nodules). A statistical analysis based on those predefined efficacy/safety end points was done and somewhat surprisingly, the authors then conclude that from an efficacy/safety perspective, D+A/BPO treatment is not inferior to ISO (74.3% vs. 58% of success, respectively).
Some other limitations:
The treatment groups forgo the possibility of observing independent effects of topical ADA+BPO, as it is combined with doxycyclin. However, there are references showing that combination of Epiduo with tetracyclines is better than tetracyclines alone.
Also, the study was done in a 85% male population, making it difficult to conclude on effects in females.
So in conclusion, I think the authors may have had some vested interest to show that the topical is non-inferior to isotretinoin. Otherwise one could have chosen a composite score equally weighted for efficacy and safety.
Article to selected by Saurat JH, MD